Is NICU Care Unnecessary for Some Premature Infants?
Findings reported this month in Pediatrics add to the evidence suggesting that neonatal intensive care units (NICUs) may be overused. Routine NICU care for low-acuity premature infants may be unnecessary and have a negative effect on breastfeeding, conclude the authors.
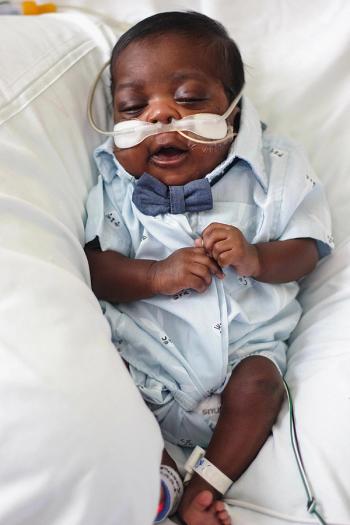
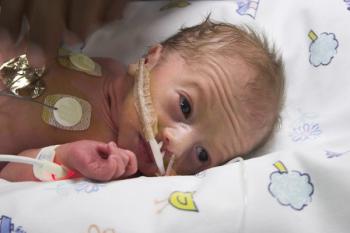
More than half (56%) of infants born at 35 weeks gestation are admitted to neonatal intensive care units (NICU). But is that precaution always medically needed — and could it cause harm among America’s 75,000 such early arrivals each year?
Even with rates of 20% for some areas, the number of NICU admissions has been increasing across all birth weights. That is “raising concern about NICU overuse,” said
Factors fueling such concerns include a California study showing that 34.5% of NICU admissions were for mild conditions, “and that hospitals with more NICU beds had an increased likelihood of NICU admissions,” she said.
To learn if rising NICU care for babies born at 35 weeks gestation is needed, Wickremasinghe and her colleagues studied chart data for 5,929 premature babies born from 2011 to 2021 at 13 Kaiser Permanente Northern California hospitals. They reported
A normal pregnancy can range from
The study excluded premature babies with congenital anomalies or who needed antibiotics or respiratory support within two hours of birth. Instead, researchers focused on the remaining 15% of babies born at 35 weeks gestation.
Researchers found significant tradeoffs for those cared for in the NICU out of what they determined was “likely discretionary or hospital policy.”
Babies in NICU were hospitalized 58 hours longer than other newborns, and babies admitted to NICU within two hours of being born were over three times more likely (67% vs. 21%) to be hospitalized for four days or longer.
On the other hand, the babies taken care of the NICU babies were half as likely (3% vs. 6%) to be readmitted within a month of being discharged.
The study said many readmissions were for “transient conditions that are more prevalent in the first week after birth.” Those include jaundice (74.6%), hypothermia and failure to thrive.
“Many of these morbidities are mild and could be managed in a mother/baby unit,” Dr. Wickremasinghe said. Such babies then could benefit from being with their mothers versus being isolated in NICU.
Mothers are affected, too. Those with infants in NICU “were more likely to be stressed, depressed and anxious, all of which impact breast milk production” and, ultimately, the bonding created by breastfeeding.
By contrast, infants staying with their mothers instead of going to NICU caused less emotional and financial stress for their families.
The takeaway from Wickremasinghe and her colleagues: “Routine NICU admission may be unnecessary for low-acuity infants born at 35 weeks’ gestation.”
Newsletter
Get the latest industry news, event updates, and more from Managed healthcare Executive.