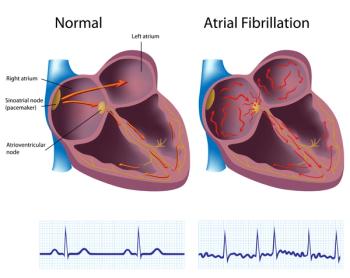
Study Provides Some Clues on How Smoking Might Lead to Atrial Fibrillation
In mouse and other studies, University of South Florida researchers traced the effects of cigarette smoke on cardiac acetylcholine-activated inward rectifier potassium current, known as the heart’s 'pacemaker.'
As evidence piles up that cigarette smoking is an independent risk factor for atrial fibrillation (AF), a new
Smokeless tobacco products are on the rise, but the Centers for Disease Control and Prevention says that
Using mouse models and human cell cultures, molecular pharmacologist Bojjibabu Chidipi, Ph.D., and his fellow investigators at the University of South Florida evaluated the downstream effects of cigarette smoke on cardiac acetylcholine- activated inward rectifier potassium current (IKACh), known as the heart’s “pacemaker.” IKACh is more active in cases of persistent AF.
According to results they reported in the journal
In mice exposed to cigarette smoke, incidents of AF were significantly longer, as measured by the time it took them to revert to normal heart rhythm following a stimulus, compared with mice that were not exposed to cigarette smoke.
To test the role of cigarette smoke on IKACh levels, investigators used tertiapinQ, a 21 amino acid synthetic peptide that is known to inhibit IKACh in AF. “Our experiment here, where tertiapinQ abrogated the effects of smoking on AF, is in line with our hypothesis that the arrhythemogenic atrial modeling induced by cigarette smoke includes an aberrant regulation of IKACh,” they wrote.
Investigators found that cell cultures exposed to extracts of cigarette smoke expressed higher levels of the IKACh-influencing Kir3.1/Kir3.4 proteins.
Cell cultures also demonstrated more abundant levels of another smoking gun in irregular IKACh function: Arf6. To confirm this upstream effect on IKACh, investigators applied NAV2729, a small-molecule selective inhibitor of Arf6.
They observed that this “abrogated the increase in IKACh brought about by 48-hour exposure” to cigarette smoke.
Based on their findings, investigators postulated that cigarette smoke activates Arf6 and thereby increases expression of Kir3.1/Kir3.4 proteins and stimulates phosphatidylinositol 4,5-biphosphate kinase (PIPK) signaling. This, in turn, increases PIP2 levels and increases IKACh, resulting in prolonged bouts of AF, they theorized.
They concluded their work helps to chip away at what has yet to be discovered about the mechanisms of AF. “Beyond the elegant studies that investigated the effects of nicotine on atrial fibrosis, there is a paucity of knowledge on how cigarette smoke modifies the atrial electrophysiological substrate,” they wrote.