Six Facts About Autoimmune Conditions Health Execs Should Know
There has been an increase in the number of people with autoimmune diseases. Here’s what you should know about them.
Approximately 50 million Americans have autoimmune diseases. Over the past two decades, there has been an increase in the number of people with these conditions.
“The reasons for this increase are not understood, but may be related to the longer-life expectancy and improved ability to diagnose autoimmune diseases,” says Anca D. Askanase, MD, MPH, associate professor of medicine and director of
Virginia Ladd, president of the
Here are six more things health executives should know about autoimmune diseases.
1. Why autoimmune conditions develop
Autoimmune diseases occur when the body’s immune system starts attacking parts of the body, such as the joints, blood vessels, lungs, kidneys, liver, and eyes. Genetic disposition and environmental factors play a role, but the disease process is not completely understood, says Shailendra Singh, MBBS, FACP, medical director of rheumatology at
2. People who have one autoimmune condition tend to develop other autoimmune conditions
“This occurs because if the immune system is not functioning properly, then more than one organ can be affected over time,” says Christopher Parker, DO, chief, Rheumatology and Clinical Immunology at
Related article:
Furthermore, autoimmune conditions tend to run in families, but children don’t always have the same diseases as other relatives. For example, a woman might have lupus, her daughter might have skin psoriasis, and her grandchild might have type 1 diabetes. And just because someone has a genetic factor for an autoimmune condition doesn’t mean they will get one, Ladd says. Something needs to trigger an autoimmune response.
3. Autoimmune conditions can range from mild to life threatening
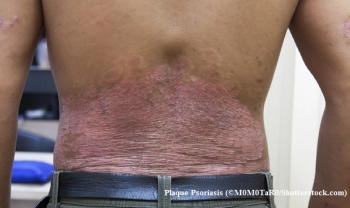
Skin psoriasis, for example, can cause a few mild patches of scaly skin or it can become very severe and affect 90% of the body, Ladd says. It can also develop into psoriatic arthritis that affects the joints. Some autoimmune conditions can become life threatening, especially if they don’t get diagnosed before major damage to organs has occurred. Many of these diseases don’t have a treatment that can stop disease progression.
Autoimmune conditions tend to have periods where they flare up or are in remission, such as skin psoriasis, psoriatic arthritis, multiple sclerosis, lupus, Crohn’s disease, rheumatoid arthritis, and Sjogren’s syndrome, Ladd says. They can also have different forms, such as relapsing-remitting multiple sclerosis, which has periods of partial or complete recovery, or progressive multiple sclerosis, which doesn’t remit.
4. Early diagnosis is difficult
One reason is because symptoms can mimic many different diseases. A patient may need to see multiple physicians depending on their symptoms, such as a dermatologist for a rash, a rheumatologist for joint involvement, and a gastroenterologist for bowel issues. It takes an average of four years to get diagnosed, Ladd says.
5. Some populations are more susceptible to autoimmune conditions
6. Autoimmune diseases have different effects on pregnancy
Some autoimmune conditions actually get better during pregnancy and some worsen, Ladd says. For example, rheumatoid arthritis can improve during pregnancy and even remit to where the patient feels quite well, while lupus can get worse.
Autoimmune conditions are associated with a higher risk of complications during pregnancy including increased risk of miscarriage, intrauterine growth retardation, fetal deformities (sometimes due to the medications used for treatment of an autoimmune condition), still births, and increased risk of maternal complications during birth, Singh says.
Newsletter
Get the latest industry news, event updates, and more from Managed healthcare Executive.