Five Ways to Reduce Costs for Patients with Autoimmune Conditions
Autoimmune patients suffer a variety of comorbidities and often require extra care-here’s how the costs of that care can be reduced.
The cost of treating autoimmune disease in the United States exceeds $100 billion annually, and that figure is likely understated, the
Here are five suggestions on how to reduce costs of care for patients with these conditions.
1. Coordinate care
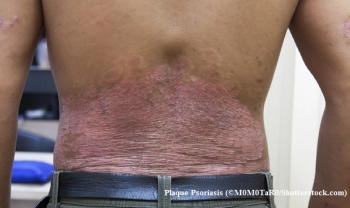
Patients with autoimmune conditions often have symptoms that require treatment from multiple physicians. For example, a patient with skin psoriasis may need to see a dermatologist for skin flares and a rheumatologist if they also have psoriatic arthritis, which 25% of skin psoriasis patients get.
Related article:
If they see physicians at different facilities, there can be gaps in care and they may have different doctors prescribe the same diagnostic testing, says Virginia Ladd, president of the
“Autoimmune diseases can be particularly challenging with no singular test to diagnose most disease types. Symptoms can also change over time as the disease manifests itself in different ways,” says Susan Manzi, MD, MPH, chair of
2. Provide diagnosis and treatment early
Studies show that if a patient is diagnosed early with an autoimmune condition and treated appropriately, it is less likely that permanent damage will occur and sometimes less expensive therapies will be effective in the early window, says Lynn Ludmer, MD, chief, Division of Rheumatology at
Unfortunately, patients aren’t always diagnosed and treated quickly due to insurance companies causing delays. Some insurers resist approving diagnostic testing such as MRIs, which may be needed to assess damage or active inflammation and can help identify patients who require more aggressive treatment regimens. Patients may forgo medications for a month or longer waiting for prior authorizations, while physicians write letters, make phone calls, and schedule peer-to-peer reviews often with physicians who practice in another specialty. “This process detracts from physicians’ ability to care for patients,” Ludmer says.
“Streamlining the approval process for medications would help significantly,” says Erin L. Arnold, MD, partner at
3. Address other risk factors
Patients with skin psoriasis and psoriatic arthritis have higher rates of smoking and being obese. Addressing these comorbidities can reduce their risk of cardiovascular disease, which is associated with these two conditions, Arnold says.
Incentive programs to help smoking cessation and weight loss would benefit these patients, Ludmer says. For example, she recommends offering partial rebates in gym memberships and smoking cessation and weight loss program fees if a patient shows up to attend sessions.
Related article:
Immunosuppressed patients are at risk for serious infections, so covering vaccines for shingles, pneumonia, and influenza at the younger end of approved guidelines such as shingles vaccines at age 50 years rather than age 60 in immunosuppressed patients or coverage for high-dose flu vaccines in all patients on immunosuppressive medications like methotrexate can save healthcare dollars by reducing the costs of hospitalizations and medications for these preventable illnesses.
4. Provide better coverage for certain medications
Some older generic medications used for rheumatoid arthritis and lupus-such as hydroxychloroquine and leflunomide-have become quite expensive, even though there aren’t any less-expensive alternatives. “It would be helpful if insurers covered those drugs at a lower tier, which could improve compliance,” Ludmer says. Improved compliance with these cheaper medications would help control disease and make it less likely that patients would request expressive biologic medication which often have copay cards available.
Related article:
Vitamin D and folic acid have been shown to help autoimmune disease, but oftentimes insurers don’t cover the prescription strength because they’re vitamins. “Taking these vitamins are inexpensive ways to help control disease and reduce the toxicity of methotrexate-which many rheumatoid arthritis patients take; perhaps they could be covered for certain conditions,” Ludmer says. “Likewise, tests to monitor drug levels of hydroxychloroquine and methotrexate levels can be costly to the patient, but if they were covered in full physicians could gauge adherence to therapy rather than adding or switching to more expensive drugs.”
5. Educate patients
If a physician or staff member educates a patient about their illness, they might be more compliant with taking their prescribed medications and presumably have better outcomes, Arnold says. Discussing the potential comorbidities and risks for side effects may compel patients to make beneficial lifestyle changes.