|Slideshows|October 19, 2018
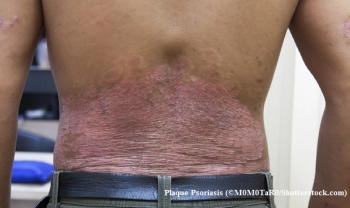
Six Ways Psoriasis Costs Extend Well Beyond Treatment of One Condition
Author(s)Karen Appold
Individuals with immune-mediated diseases, such as psoriasis, are at higher risk for having other immune-mediated diseases. Here’s how psoriasis can lead to other conditions, and the associated costs.
Advertisement
Newsletter
Get the latest industry news, event updates, and more from Managed healthcare Executive.
Advertisement
Latest CME
Advertisement
Advertisement
Trending on Managed Healthcare Executive
1
7 things you need to know about the PBM reforms signed into law this week
2
PBM reform. It has finally happened
3
Cancer survival fell and deaths rose during first two years of COVID-19
4
TrumpRx launches; some experts question its long-term value
5