Oxygen for Newborns: When There Is Too Much of a Necessary Thing
Oxygen supplementation may be necessary, especially for newborns born prematurely. But the oxygen free radicals associated with high levels can be harmful, causing conditions such as retinopathy of prematurity, which can result in blindness. A review article discusses how researchers and clinicians have found the right balance between high and low oxygen supplementation for newborns.
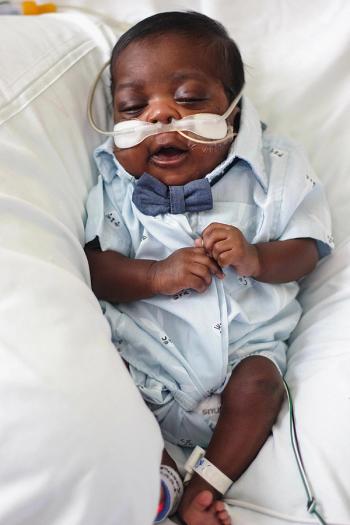
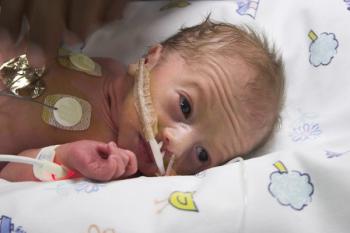
Oxygen supplementation is often a critical part of neonatal care. Newborns, especially those born prematurely, may need oxygen supplementation during resuscitation and for stabilization afterward.
But exposure to high levels of oxygen can also have as a byproduct the generation of tissue-damaging “oxidative stress” if unstable reactive oxygen-containing molecules — also called oxygen free radicals — get too high. Oxygen supplementation is also associated with the creation of unstable nitrogen-containing molecules, such as nitric oxide and peroxynitrite, that can damage a variety of tissues.
In a
“Despite recent clinical studies, oxygen can still be considered a double-edged sword since higher levels may increase survival, although with increased risk of severe sequelae,” they wrote.
Vitamin E is an antioxidant that “soaks up” oxygen free radicals but, but Perrone and her colleagues note that data from clinical trials of vitamin E supplementation in preterm infants provided little supporting evidence for the supplementation.
The 17-page review article discusses some of the back-and-forth about the optimum levels of oxygen supplementation and the trade-offs between high and low levels.
In 1992, the American Heart Association guidelines for newborn resuscitation said that “100% oxygen should be used, it is not toxic and there are no reasons to be concerned,” according to Perrone and her colleagues.
But the review also notes that the potential toxicity of oxygen was identified in the early 1950s by
Here some of the other conditions related to oxygen and oxidative stress discussed in the review:
Bronchopulmonary dysplasia is a major cause of chronic lung disease and morbidity in preterm infants. The review says one of the main causes of the condition is oxidative stress sustained by inflammation due to exposure to high oxygen levels (“hyperoxia exposure”). High oxygen levels may spur on fibrotic process in lung tissue and interfere with the production of surfactant, a mixture of fats, proteins and carbohydrate that coats lung tissue and keeps them functioning.
Necrotizing enterocolitis is a potentially life-threatening condition characterized by inflammation and bacterial invasion of the wall of the large intestine. Some researchers have proposed that it is at least partially caused by inability of epithelial cells in the gut to cope with oxidative stress.
Studies conducted in the mid-20th century showed that more limited use of oxygen resulted in fewer deaths, decreased respiratory failure and decreased lung disease, according to the Perrone and her co-authors. But researchers and clinicians also had to weigh the evidence reduced oxygen supplementation was associated with a higher risk of cerebral palsy. The review cites
That was far from the last word, though, as researchers continued to try to figure out the safest and most effective oxygen level. Results from the Supplemental Therapeutic Oxygen for Prethreshold-ROP (STOP-ROP) study showed that high levels of oxygen did not prevent the progression of ROP but were associated with pneumonia, chronic lung disease and hospitalization.
A definitive meta-analysis called the Neonatal Oxygen Prospective Meta-Analysis (NeOProM) that was published in 2011 in the BMC Pediatrics concluded there was no difference in death, disability and neurodevelopmental impairment, such as cerebral palsy or cognitive impairment, between high- and low-exposure oxygen groups. But this meta-analysis showed again that there may be some tradeoffs: low oxygen saturation (the proportion of hemoglobin bound to oxygen) was associated with 25% reduced risk of ROP, according to the meta-analysis but a 25% increase in necrotizing enterocolitis.
Perrone and her colleagues say results from STOP-ROP and NeOProM studies suggested a mid-range target level for oxygen saturation.
“Extreme excess supplementation of oxygen is not administered in modern NICUs (neonatal intensive care units),” they wrote in the review article. “This means that ROS (reactive active species)-mediated injuries due to hyperoxia may be reduced in the recent era.”